Background
In 2019, a uniquely inclusive expert clinical and community panel was formed to better understand the nature of prostate cancer survivorship and to identify survivorship domains and domain elements for inclusion in care guidelines taking into account evidence, importance, feasibility and consensus. The initiative resulted in the identification of domains that extend beyond traditional healthcare parameters to provide guidance for policymakers, clinicians, community and consumers on what is essential for step change in prostate cancer survivorship outcomes.
The 47-member panel included leaders from key Australian and New Zealand clinical and community groups and consumers from diverse backgrounds, including LGBTQIA people and those from regional, rural and urban settings.
Panel members included urologists, medical and radiation oncologists, family doctors, nurses, and physiotherapists from organisations including Cancer Council Australia, Peter MacCallum Cancer Centre, Cancer Voices New South Wales, Prostate Cancer Foundation of Australia, Prostate Cancer Foundation of New Zealand, Urological Society of Australia and New Zealand, Australian Prostate Centre.
The panel reached the view that improving the quality of prostate cancer survivorship requires a high care focus on the wider psychosocial impacts of cancer as well as medical intervention.
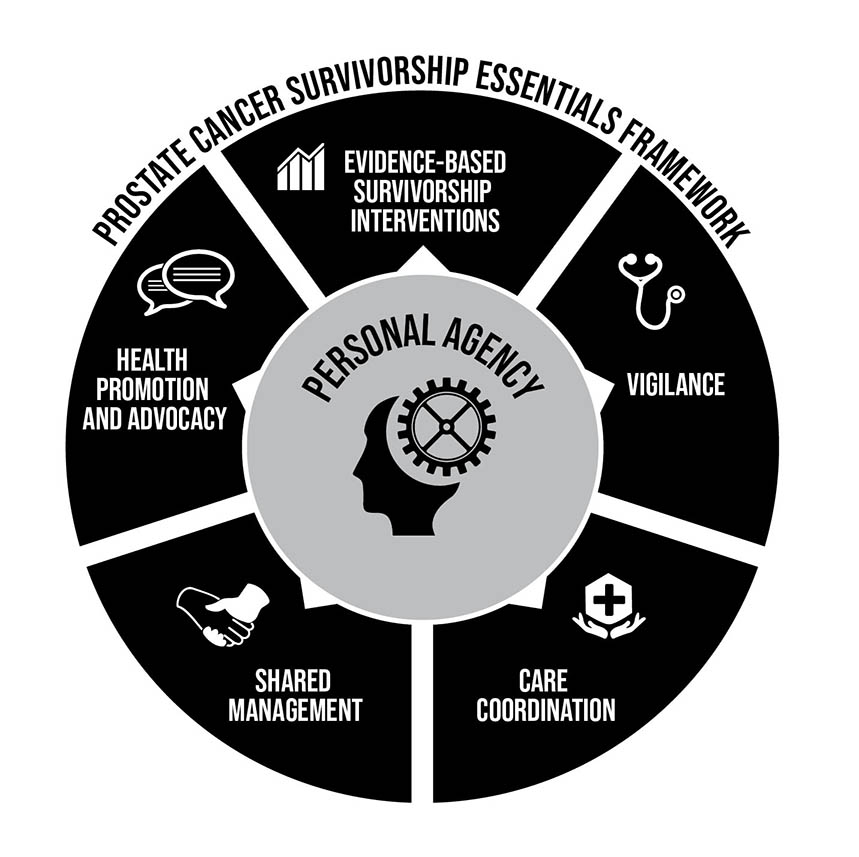
Six essential aspects of survivorship, including the vitally important component of personal agency, were identified:
- Health Promotion and Advocacy
- Shared Management
- Vigilance
- Personal Agency
- Care Coordination
- Evidence-based Survivorship Interventions
The Framework in Use
The world’s first use of the Framework in a patient care resource was in 2020, when the new edition of Facing the Tiger was released with a new chapter outlining what the framework means to men, their partners and their health care team. It shows how a focus on personal agency contributes to a better quality of life in survivorship.
In September 2021, a A$2.25 million funded translational research trial was announced in Australia based on the Prostate Cancer Survivorship Essentials Framework to inform health service delivery in a real-world setting. The trial tests the clinical and cost-effectiveness of nurse-led survivorship care for improving the health and well-being of men on hormone therapy for prostate cancer. It covers 200 men, with care provided by around 100 specially-trained prostate cancer care nurses through telehealth sessions. Nurse training uses The Health Professionals Guide to Delivering Psychological Care for Men with Prostate Cancer, with patient support resources anchored by Facing the Tiger. While the trial is still underway, published results of a small qualitative exploratory study in 2025 suggests that delivery of the telehealth program is highly acceptable to participants, and to the nurses delivering it. (https://www.ejoncologynursing.com/article/S1462-3889(25)00060-2/fulltext). This is an important first step in using the Framework to establish a sustainable tailored care model and bring better understanding of how specialised support improves quality of life and survivorship outcomes for men on hormone therapy.
In 2023 the Framework was modified to encompass a wider approach for all cancers via the Cancer Survivorship Essentials Framework. Following on the principles established in The Health Professionals Guide to Delivering Psychological Care for Men with Prostate Cancer, a new health professional’s manual was released called The Health Professionals Guide to Delivering Psychological Care for Adults with Cancer which uses a series of online accessible patient resources instead of a stand alone patient book.
In 2025, nurse training is being conducted for Lung Foundation Australia nurses using the The Health Professionals Guide to Delivering Psychological Care for Adults with Cancer, while Facing the Tiger continues to be used by groups such Mens Health Downunder, Brisbane Urology Clinic, and PCFA.
The Future
Survivorship matters to all. Research shows that cancer patients and their doctors, and the nurses and allied health professionals who look after them, report the experience of cancer as being challenging, medically focused, and uncoordinated, with patient’s support needs often not being adequately met. It makes sense then, to use both the Prostate Cancer Survivorship Essentials Framework and the Cancer Survivorship Essentials Framework to guide modern treatment for cancer. Ensuring a psychosocial as well as medical focus throughout treatment brings with it better survivorship.